Your Cart is Empty

Got arthrosis? Or just curious about what it is? As a condition affecting around 30 million people in the U.S. alone, it’s not uncommon and may just impact more people than you might guess. If you break that down that’s 600,000 individuals for each state in the Union (that number exceeds the population of Wyoming!). You might even be affected by arthrosis yourself.
Often mistakenly called “arthosis”, this condition is actually called arthrosis with an “r” thrown in after the “h”. To make things even more complicated, there is also a disease known as atherosclerosis(aka arthrosclerotic cardiovascular disease -- now there’s a mouthful!), which sounds very similar but affects the heart and arteries. So, now that we’ve got that little bit of confusion cleared up, let’s take a closer look at arthrosis.
What is arthrosis? Is it the same as arthritis? Arthrosis sounds a lot like “arthritis” -- so is this just a coincidence? Not at all! Arthrosis isa type of arthritis, specifically the form typically called osteoarthritis (OA). You may have also heard it referred to as degenerative joint disease or degenerative arthritis.
The term “arthrosis” is more commonly used in Europe, whereas, here in the U.S. we often use the term “osteoarthritis” to describe the condition.
As if all of these similarities aren’t overwhelming enough, it becomes even more complicated when you start trying to separate out the differences in arthritis types. This is where it is especially helpful to understand what arthritis is and how your particular form can affect you.
Arthritis isn’t a condition unto itself, but rather a blanket term that’s used to describe several different pain conditions that can occur in the body. This vast group includes arthrosis (also called osteoarthritis or OA), fibromyalgia, rheumatoid arthritis (RA), childhood arthritis, lupus and gout.
Because of the many different masks that arthritis can wear, it’s important that you are able to differentiate between the numerous types to get the best and most effective relief from your symptoms.
 Unlike some other forms of arthritis, arthrosis affects only the structure of the joints and the immediately surrounding soft tissues. It causes inflammation, which in turn makes your nerves in the area pretty angry. The result? Pain and sometimes swelling.If you’ve been diagnosed with arthrosis (OA) you are probably already aware that is the most common type of arthritis to affect adults over the age of 18, but it is especially prominent in women aged 60 and older.
Unlike some other forms of arthritis, arthrosis affects only the structure of the joints and the immediately surrounding soft tissues. It causes inflammation, which in turn makes your nerves in the area pretty angry. The result? Pain and sometimes swelling.If you’ve been diagnosed with arthrosis (OA) you are probably already aware that is the most common type of arthritis to affect adults over the age of 18, but it is especially prominent in women aged 60 and older.
Your joints are complex. They consist of bones that are perfectly shaped to work together. Between these bones is a layer of rubbery, smooth tissue known as cartilage.
The cartilage in your joints is literally about as tough a car tire. It creates a somewhat slick surface (this is where synovial fluid comes in -- we’ll cover that in the future) that allows your bones to move effortlessly together.
The disconnect (so to speak) happens when this cartilage becomes damaged.
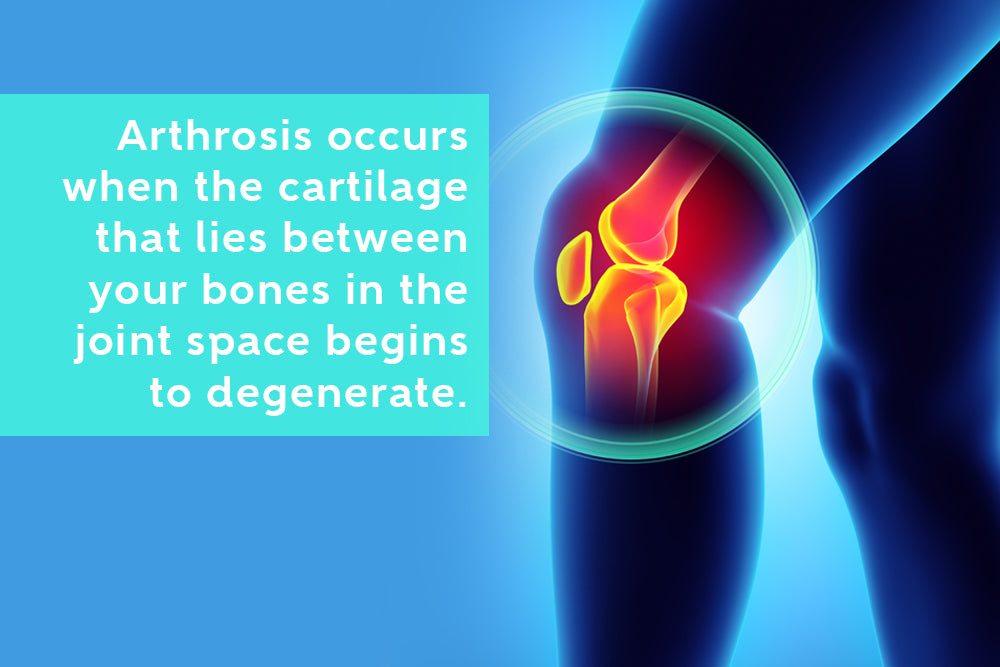
To break it down even further (no pun intended), arthrosis occurs when the cartilage that lies between your bones in the joint space begins to degenerate. There are numerous things that can contribute to the development of arthrosis.
Bone spurs, which are small, benign growths of bone tissue can grow on and around your joints. They’re a double-edged sword, in that they may develop in response to arthritic changes, making things even worse. This is a fairly common cause and symptom of arthrosis.
The most common cause of arthrosis is the normal wear and tear on your joints that occurs with aging.
Everyday, you are putting pressure and stress on your joints. The cartilage in your joints is there to help cushion the impact and protect the bones from one another. Over time, this protective layer between your bones starts to wear away.
In the absence of a healthy padding of cartilage, the bone-on-bone contact is what causes that pain, grating and stiffness you may be experiencing.
We all blame our parents for lots of stuff. They may not have given you that pony for your tenth birthday but they could have unknowingly gifted you with genes that predispose you to arthrosis.
Arthrosis can run in families, with arthritis-causing genetics being passed down to each new generation. Like a game of Russian roulette, you may develop arthrosis thanks to these genes while your siblings might not.
You’ve probably heard people complain about old sports injuries and the subsequent pain they cause long-term.
In some cases these complaints could be due to soft tissue damage but in many instances it’s all because of the arthritic changes that happen in the damaged joints. Injury-related arthrosis is fairly common and can occur in any joint in the body.

Being overweight or obese is also a major cause of osteoarthritis -- particularly in the knees and hips. An estimated 72.5 million people over the age of 20 years in the U.S. alone are obese.
As that extra weight pushes down on the joints, it can cause premature wear to the cartilage.
The joints that are affected most severely by extra body weight are the knees and hips. Both take the brunt of the daily impact we exert on our bodies.
Maintaining a healthy weight for your frame and lifestyle is essential to help preserve your joints and keep arthrosis at bay.
Exploring different diet options and losing weight (if you’re carrying around those extra few pounds) could help make the difference between keeping your joints in tiptop shape or having to contend with arthrosis (among many other health issues).
We’ve already explored some of the mechanics and causes of arthrosis, but just where in the body does it commonly occur? Obviously, the knees and hips, as mentioned earlier, but it can literally occur in any joint in the body.
Here’s a closer look at the different points in your body where it might develop.

Acromioclavicular joint arthrosis may sound Mary Poppins-like with an almost nonsensical lengthiness to the words, but it’s no laughing matter.
The acromioclavicular joint is located in your shoulder (also known as the “ac joint” for short). It essentially creates the connection between your collarbone (clavicle) and shoulder blade (scapula).
This may seem like an odd place for a joint; by all appearances there is nothing but muscle and soft tissue in your upper shoulders. Ironically, acromioclavicular joint arthrosis can be one of the most painful and debilitating.
Those that put a lot of wear and tear (such as weight lifters or construction workers) are the most commonly affected by this type of arthrosis.
Injuries of this joint such as car accidents, falls or anything that puts undue stress on the shoulder area can also lead to AC joint arthrosis.
In addition to the loss of cartilage, AC joint arthrosis tends to develop bone spurs which can wear on the cartilage and put pressure on soft tissue and nerves in the area. These spurs can also limit mobility and make even raising your arms above your head difficult.
Some of the symptoms that are commonly experienced with acromioclavicular joint arthrosis include clicking or popping noises, a loss of flexibility and mobility and pain or tenderness.

Perhaps the most common of the arthrosis types, knee arthrosis affects a wide range of people. Because your knees take the majority of stress and impact from your body’s movements, they are highly susceptible to becoming arthritic.
In most cases, knee arthrosis is due to the normal stress placed on your knee joints. People that spend a lot of time on their feet (such as mail carriers or factory workers) may find they experience knee arthritis later in life.
If you’re a hard-hitting athlete, you may find that your knees are more prone to aches and pains -- this may be the beginnings of arthrosis.
When looking at knee arthrosis, you can expect to have pain that increases with activity. Stiffness and difficulty moving your knees through their entire range of motion may also be indications of osteoarthritis in your knees.
If you’ve been experiencing chronic lower back aches, don’t automatically assume that it’s due to a ruptured disc or pulled muscle.
As the part of your back that absorbs the majority of weight and impact, the discs and cartilage can experience the same strains other joints in your body can.

Lumbar arthrosis is typically associated with an excess of weight being carried in the abdominal region (a pot belly) or poor posture that pushes your entire spine into an abnormal position.
With lumbar arthrosis you may experience pain in your lower back that is at its worst when you’re upright but is relieved by lying down. Many people also report that they have difficulty bending over or stooping down due to pain and decreased flexibility.

Have you ever heard of “facets” in your spine? They’re the tiny joints that lie between the vertebrae in your back and run along the spinal cord. Even these joints are not excluded from arthrosis.
Facet arthrosis is caused mainly by age-related wear and tear but can be exacerbated by bad posture.
Typically found in older people, facet arthrosis creates pain that can range along the entire spine.
Seriously, arthrosis will happen anywhere. The next up is the neck. Affecting the cervical vertebrae (the bones of your neck), this painful version is typically due to aging and the stress and wear placed on that region of your spine.

Cervical arthrosis comes with a full menu of symptoms, including tension headaches, neck pain, stiffness or difficulty moving your head in a full range of motions and even muscle spasms and stiffness that can extend down into your upper shoulders and back.
Last, but not least, we come to coxarthrosis. This form of arthritis is responsible for much of the hip pain and dysfunction experienced by seniors.

Coxarthrosis occurs in the hip joint. This is where the ball fits into the socket, giving you that full range of motion.
Use and normal wear and tear can lead to the development of this arthrosis, but anyone that uses their hips extensively (such as athletes) can experience arthrosis of the hip.
A good indication that you may be suffering from coxarthrosis is if you’re experiencing hip pain that is most prominent when you’re in an upright position. Other symptoms can include a grinding sound with certain movements and a reduced range of motion.
Like any condition, treating arthrosis doesn’t come with a one-size-fits-all solution. Depending on the advancement of your arthrosis and other factors like your age, you may find some treatments work while others don’t. Luckily, there is a wide range of things you can do right at home to help ease the pain and discomfort of your arthrosis.
Over-the-counter (OTC) and prescription NSAIDs are one of the first treatments people try when dealing with the pain and discomfort of arthrosis.
While these drugs may offer varying levels of temporary relief, they come with a whole raft of side effects many find unbearable.
A longer-lasting option, steroidal injections are often used to reduce inflammation associated with arthrosis.
They are frequently injected into the joints or soft tissues such as tendons surrounding the joint, keeping inflammation at bay.
Although opioids can be a good short-term solution for acute pain (such as immediately following surgery or major injury), they carry with them some pretty heavy risks.
Narcotic drugs are highly addictive and often require increasingly larger doses to achieve relief from pain and discomfort.
Another unwanted side effect from opioids is a slowing of peristalsis (the process by which the intestines move waste out of the body), resulting in constipation and even potentially life-threatening conditions if left untreated.
There is a tremendous amount of research taking place around natural compounds to treat arthrosis, and in some cases even restore the lost cartilage.
Glucosamine and chondroitin are both promising on their own but together provide an incredibly potent joint treatment. They work well either ingested or used transdermally, making them a great option for a wide number of people.
Turmeric has gained popularity amongst those seeking a safer option to pharmaceuticals. Used for thousands of years for a wide variety of health complaints, it now has modern science to back its efficacy, especially when used for inflammation.
Other dietary supplements that are proving effective in the fight against the ravages of arthrosis include MSM, magnesium and aloe vera, just to name a few.
Remember that terrible-smelling liniment your grandparents would rub into their aching joints? It may have seemed like voodoo but there was probably something to it.
Luckily, science has allowed us to better formulate and standardize these topicals and transdermals, making them all the more effective.
Topicals and transdermals are a fantastic option, in that they’re highly portable and can be used anytime and anywhere.
So what’s the difference between the two?
Topicals are just that -- they stay on the surface of the skin and impart subtle effects.
Transdermals, on the other hand, provide a higher level of therapeutic efficacy. They penetrate the skin and allow their ingredients to be carried to the affected area.
Of course, when using a transdermal it’s vital to make sure it doesn’t contain scary chemicals or other harmful substances that could negate all of the good stuff or introduce unwanted ingredients into your body.
It’s long been known that if you sit around you will only make your joints stiff and increase the pain you experience.
It might seem counterintuitive to get up and exercise; after all, your joints likely got to the place they’re at from use.
Interestingly, it’s the opposite -- your joints will stay more flexible and you’ll be able to maintain a greater range of motion with gentle exercise.
Flexibility is one of the biggest issues with osteoarthritis. When you have arthrosis your joints may begin to “seize up” if they’re not run through stretching and flexibility exercises to help you maintain your range of motion.
Secondly, without adequate strength training, the muscles surrounding your joints can begin to atrophy. This may seem unrelated but when you think about it, strong muscles help to support joints and can reduce additional wear and tear.
Cardio is also essential. Now that one seems truly weird, right? Well, having a healthy circulatory system can help to deliver fresh oxygen and nourishment via your bloodstream to your joints, while carrying away damaged cells and inflammatory by-products.
Lastly, exercise helps regulate your metabolism, which in turn helps you burn calories. As mentioned before, obesity is one of the largest contributors to the development of arthrosis, making weight control essential in the fight against arthritis. Regular exercise can help you not only maintain an optimum weight, but if you are overweight, it can aid in weight loss.

Low-impact exercise is obviously necessary to prevent further joint damage. Many physical therapists and chiropractors recommend activities such as swimming -- this allows for a wide range of motion with little-to-no impact being placed on the joints themselves.

In cases where you are experiencing a great deal of pain or immobility due to arthrosis, you may want to seek the help of a physical therapist (PT). Highly trained in helping people regain strength and mobility from a wide variety of injuries and conditions, a PT will be able to develop a treatment plan for you that addresses your unique needs.
Finding relief for your arthrosis shouldn’t be a stressful undertaking. With the wide variety of treatments available, you can find the perfect combination for your unique needs.